Abstract
Background
Cancer therapies that target the PD-1/PD-L1 pathway are in ongoing phase I/II clinical trials for several tumor types. However, the prognostic value of PD-L1 expression in breast cancer is unclear.
Objective
We assessed the prognostic role of PD-L1 expression in breast cancer.
Methods
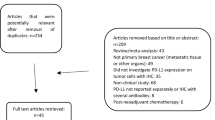
We searched Medline/PubMed for eligible studies of the association between PD-L1 expression and patient survival in breast cancer published before 7 December 2015. The effect size was the hazard ratio (HR) with 95 % confidence interval (CI) for overall survival (OS), recurrence-free survival (RFS) and metastasis-free survival (MFS). Odds ratios (OR) with 95 % CIs were also extracted to evaluate associations between PD-L1 expression and patient clinicopathological features.
Results
We included five studies with 7,802 total patients in this meta-analysis. The pooled OR associated high PD-L1 expression with predictors of poor-prognosis: high tumor grade, negative ER status, negative PR status, positive HER2 status and lymphovascular invasion. High PD-L1 protein expression was associated with shorter OS (HR = 3.22, 95 % CI: 1.86–5.59; P < 0.0001), shorter RFS (HR = 1.38, 95 % CI: 1.03–1.86; P = 0.03) and shorter MFS (HR = 3.33, 95 % CI: 2.30–4.82; P < 0.00001); whereas high PD-L1 mRNA expression was associated with longer OS (HR = 0.86, 95 % CI: 0.75–1.00; P = 0.05) and longer RFS (HR = 0.57, 95 % CI: 0.36–0.91; P = 0.02).
Limitations
The findings of these studies were significantly heterogeneous; the results should be interpreted cautiously.
Conclusion
In breast cancer, high PD-L1 protein expression appears to be a negative prognostic factor, whereas high PD-L1 mRNA expression appears to be a favorable prognostic factor.






Similar content being viewed by others
References
Pennock GK, Chow LQ. The evolving role of immune checkpoint inhibitors in cancer treatment. Oncologist. 2015;20:812–22.
Sakaguchi S, Wing K, Onishi Y, et al. Regulatory T cells: how do they suppress immune responses? Int Immunol. 2009;21:1105–11.
Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer. 2012;12:252–64.
Flies DB, Sandler BJ, Sznol M, et al. Blockade of the B7-H1/PD-1 pathway for cancer immunotherapy. Yale J Biol Med. 2011;84:409–21.
Whiteside TL. The role of death receptor ligands in shaping tumor microenvironment. Immunol Investig. 2007;36:25–46.
Sharabi AB, Lim M, Deweese TL, et al. Radiation and checkpoint blockade immunotherapy: radiosensitization and potential mechanisms of synergy. Lancet Oncol. 2015;16(13):e498–509.
La-Beck NM, Jean GW, Huynh C, et al. Immune checkpoint inhibitors: new insights and current place in cancer therapy. Pharmacotherapy. 2015;35:963–76.
Ghasemzadeh A, Bivalacqua TJ, Hahn NM, et al. New strategies in bladder cancer: a second coming for immunotherapy. Clin Cancer Res. 2016;22:793–801.
Chen J, Jiang CC, Jin L, et al. Regulation of PD-L1: a novel role of pro-survival signaling in cancer. Ann Oncol. 2016;27:409–16.
Ali OA, Lewin SA, Dranoff G, et al. Vaccines combined with immune checkpoint antibodies promote cytotoxic T cell activity and tumor eradication. Cancer Immunol Res. 2016;4:95–100.
Herbst RS, Soria JC, Kowanetz M, et al. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature. 2015;515:563–7.
Reiss KA, Forde PM, Brahmer JR. Harnessing the power of the immune system via blockade of PD-1 and PD-L1: a promising new anticancer strategy. Immunotherapy. 2014;6:459–75.
Gatalica Z, Snyder C, Maney T, et al. Programmed cell death 1 (PD-1) and its ligand (PD-L1) in common cancers and their correlation with molecular cancer type. Cancer Epidemiol Biomarkers Prev. 2014;23:2965–70.
Zhong A, Xing Y, Pan X, et al. Prognostic value of programmed cell death-ligand 1 expression in patients with non-small-cell lung cancer: evidence from an updated meta-analysis. Onco Targets Ther. 2015;8:3595–601.
Prall F, Huhns M. PD-L1 expression in tumor buds of colorectal carcinoma. Histopathology. 2016;69:158–60.
Liu J, Liu Y, Wang W, et al. Expression of immune checkpoint molecules in endometrial carcinoma. Exp Ther Med. 2015;10:1947–52.
Berretta M, Stanzione B, Di Francia R, et al. The expression of PD-L1 APE1 and P53 in hepatocellular carcinoma and its relationship to clinical pathology. Eur Rev Med Pharmacol Sci. 2015;19:4207–9.
Weinstock M, Mcdermott D. Targeting PD-1/PD-L1 in the treatment of metastatic renal cell carcinoma. Ther Adv Urol. 2015;7:365–77.
Thoma C. Prostate cancer: PD-L1 expression is common and indicates poor prognosis. Nat Rev Urol. 2016;13:5.
Marquez-Rodas I, Cerezuela P, Soria A, et al. Immune checkpoint inhibitors: therapeutic advances in melanoma. Ann Transl Med. 2015;3:267.
Qin T, Zeng YD, Qin G, et al. High PD-L1 expression was associated with poor prognosis in 870 Chinese patients with breast cancer. Oncotarget. 2015;6:33972–81.
Muenst S, Schaerli AR, Gao F, et al. Expression of programmed death ligand 1 (PD-L1) is associated with poor prognosis in human breast cancer. Breast Cancer Res Treat. 2014;146:15–24.
Baptista MZ, Sarian LO, Derchain SF, et al. Prognostic significance of PD-L1 and PD-L2 in breast cancer. Hum Pathol. 2016;47:78–84.
Schalper KA, Velcheti V, Carvajal D, et al. In situ tumor PD-L1 mRNA expression is associated with increased TILs and better outcome in breast carcinomas. Clin Cancer Res. 2014;20:2773–82.
Sabatier R, Finetti P, Mamessier E, et al. Prognostic and predictive value of PDL1 expression in breast cancer. Oncotarget. 2015;6:5449–64.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–69. W64.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151:W65–94.
Vandenbroucke JP, von Elm E, Altman DG, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. Int J Surg. 2014;12:1500–24.
Zeng LN, Zhang LL, Shi J, et al. The primary microbial pathogens associated with premature rupture of the membranes in China: a systematic review. Taiwan J Obstet Gynecol. 2014;53:443–51.
Malhamé I, Cormier M, Sugarman J, Schwartzman K. Latent tuberculosis in pregnancy: a systematic review. PLoS One. 2016;11, e0154825.
Tierney JF, Stewart LA, Ghersi D, et al. Practical methods for incorporating summary time-to-event data into meta-analysis. Trials. 2007;8:16.
Duval S, Tweedie R. Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics. 2000;56:455–63.
Mahoney KM, Freeman GJ, Mcdermott DF. The next immune-checkpoint inhibitors: PD-1/PD-L1 blockade in melanoma. Clin Ther. 2015;37:764–82.
Nanda R, Chow LQ, Dees EC, et al. Pembrolizumab in patients with advanced triple-negative breast cancer: Phase Ib KEYNOTE-012 Study. J Clin Oncol. 2016.
Dirix LY, Takacs I, Nikolinakos P, et al. Avelumab (MSB0010718C), an anti-PD-L1 antibody, in patients with locally advanced or metastatic breast cancer: a phase Ib JAVELIN solid tumor trial [abstract]. In: Proceedings of the Thirty-Eighth Annual CTRC-AACR San Antonio Breast Cancer Symposium; 2015 Dec 6–10; San Antonio, TX. Philadelphia (PA): AACR; Cancer Res 2016;76(4 Suppl):Abstract nr S1-04.
Emens LA, Braiteh FS, Cassier P, et al. Inhibition of PD-L1 by MPDL3280A leads to clinical activity in patients with metastatic triplenegative breast cancer (TNBC) [abstract]. In: Proceedings of the 106th Annual Meeting of the American Association for Cancer Research; 2015 Apr 18–22; Philadelphia, PA. Philadelphia (PA): AACR; Cancer Res 2015;75(15 Suppl):Abstract nr 2859.
Rizvi N, Shepherd F, Antonia S, et al. First-line monotherapy with nivolumab (anti-PD-1; BMS-936558, ONO-4538) in advanced non-small cell lung cancer (NSCLC): safety, efficacy and correlation of outcomes with PD-L1 status. J Radiat Oncol Biol Phys. 2014;90:S31.
Luis P, Horn L, Borghaei H, et al. Phase III, randomized trial (CheckMate 057) of nivolumab versus docetaxel in advanced non-squamous (non-SQ) cell non-small cell lung cancer (NSCLC). J Clin Oncol. 2015; 33(suppl), abstract LBA109.
Brahmer J, Reckamp KL, Baas P, et al. Nivolumab versus docetaxel in advanced squamous-cell non-small-cell lung cancer. N Engl J Med. 2015;373:123–35.
Rizvi NA, Mazieres J, Planchard D, et al. Activity and safety of nivolumab, an antiPD-1 immune checkpoint inhibitor, for patients with advanced, refractory squamous non-small-cell lung cancer (CheckMate 063): a phase 2, single-arm trial. Lancet Oncol. 2015;16:257–65.
Ali HR, Glont SE, Blows FM, et al. PD-L1 protein expression in breast cancer is rare, enriched in basal-like tumours and associated with infiltrating lymphocytes. Ann Oncol. 2015;26:1488–93.
Ghebeh H, Mohammed S, Al-Omair A, et al. The B7-H1 (PD-L1) T lymphocyte-inhibitory molecule is expressed in breast cancer patients with infiltrating ductal carcinoma: correlation with important high-risk prognostic factors. Neoplasia. 2006;8:190–8.
Lastwika KJ, Wrd W, Li QK, et al. Control of PD-L1 expression by oncogenic activation of the AKT/mTOR pathway in non-small cell lung cancer. Cancer Res. 2016;76:227–38.
Green MR, Monti S, Rodig SJ, et al. Integrative analysis reveals selective 9p24.1 amplification, increased PD-1 ligand expression, and further induction via JAK2 in nodular sclerosing Hodgkin lymphoma and primary mediastinal large B-cell lymphoma. Blood. 2010;17:3268–77.
Akbay EA, Koyama S, Carretero J, et al. Activation of the PD-1 pathway contributes to immune escape in EGFR-driven lung tumors. Cancer Discov. 2013;3:1355–63.
Crane CA, Panner A, Murray JC, et al. PI(3) kinase is associated with a mechanism of immunoresistance in breast and prostate cancer. Oncogene. 2009;28:306–12.
Bordeaux JM, Cheng H, Welsh AW, et al. Quantitative in situ measurement of estrogen receptor mRNA predicts response to tamoxifen. PLoS One. 2012;7, e36559.
Velcheti V, Schalper KA, Carvajal DE, et al. Programmed death ligand-1 expression in non-small cell lung cancer. Lab Investig. 2014;9:107–16.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
None.
Conflict of Interest
The authors declare no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplemental Table 1
(DOC 74 kb)
Supplemental Table 2
(DOC 101 kb)
Rights and permissions
About this article
Cite this article
Li, X., Li, M., Lian, Z. et al. Prognostic Role of Programmed Death Ligand-1 Expression in Breast Cancer: A Systematic Review and Meta-Analysis. Targ Oncol 11, 753–761 (2016). https://doi.org/10.1007/s11523-016-0451-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11523-016-0451-8