Abstract
Survival after pancreatic cancer remains poor despite incremental advances in surgical and adjuvant therapy, and new strategies for treatment are needed. Oncolytic virotherapy is an attractive approach for cancer treatment. In this study, we have evaluated the effectiveness of the Lister vaccine strain of vaccinia virus armed with the endostatin–angiostatin fusion gene (VVhEA) as a novel therapeutic approach for pancreatic cancer. The Lister vaccine strain of vaccinia virus was effective against all human pancreatic carcinoma cells tested in vitro, especially those insensitive to oncolytic adenovirus. The virus displayed inherently high selectivity for cancer cells, sparing normal cells both in vitro and in vivo, with effective infection of tumors after both intravenous (i.v.) and intratumoral (i.t.) administrations. The expression of the endostatin–angiostatin fusion protein was confirmed in a pancreatic cancer model both in vitro and in vivo, with evidence of inhibition of angiogenesis. This novel vaccinia virus showed significant antitumor potency in vivo against the Suit-2 model by i.t. administration. This study suggests that the novel Lister strain of vaccinia virus armed with the endostatin–angiostatin fusion gene is a potential therapeutic agent for pancreatic cancer.
Similar content being viewed by others
Introduction
Pancreatic cancer is currently a leading cause of cancer-related deaths in the Western countries as most patients present with advanced or metastatic disease and few are suitable for curative surgical resection. Palliative chemotherapy has poor results and the overall 5-year survival rate is <5%.1 New treatment strategies are clearly imperative. With increasing knowledge of the molecular genetics of pancreatic cancer,2 gene therapy has become an attractive option, although clinical trials to date have shown only moderate efficacy.3
Replication-selective oncolytic viruses are rapidly expanding as a class of therapeutic agents for cancer. Replication-selective oncolytic adenovirus is the most well-researched, and a first generation virus (dl1520, or H101 in China) has been approved as the world's first oncolytic virotherapy for head and neck cancer therapy.4 This virus has been administered by intratumoral (i.t.) injection into patients with locally advanced pancreatic tumors in phase I–II trials. Although treatments were well tolerated, no objective responses were seen in patients after virus alone, and only two of 21 patients showed objective responses when gemcitabine was used in combination.5 One major hurdle affecting oncolytic adenovirus potency is the genetic make-up in cancer cells, which affects virus infectivity. For example, the expression of adenovirus receptor, CAR (coxsackie-adenovirus receptor) is often low on many tumor types, including pancreatic cancer.6 To make progress, new strategies are needed to overcome this obstacle. One of them could be to the use other oncolytic viruses such vaccinia virus.
Oncolytic vaccinia virus represents an attractive alternative, as it has several features that make it suitable for use as an oncolytic agent.7, 8, 9, 10, 11 A defining feature of vaccinia virus as an oncolytic agent is that it relies mostly on its own encoded proteins to carry out replication and transcription in the cytoplasm, with few (if any) host proteins required. In addition, the vaccinia virus has a wide host range and tissue tropism, which provides an ability to infect almost all types of mammalian cells. These may overcome the difficulty encountered with adenovirus and allow vaccinia virus to replicate in many tumor types. The vaccinia virus has been safely injected into patients through subcutaneous,12 intramuscular,13 intratumoral14 and intravesical15 administration. The oncolytic capacity of vaccinia virus, as well as the safety record of this virus, make it a potentially ideal choice for cancer treatment.11, 16, 17
Oncolytic vaccinia virus is inherently tumor selective in part because of the low production of interferons by tumor cells in response to vaccinia infection, whereas these cytokines inhibit vaccinia replication in normal cells.18 However, tumor selectivity is enhanced because of the overexpression of EGFR (epidermal growth factor receptor) by many tumor types. Vaccinia viruses express vaccinia growth receptor early during replication. Vaccinia growth receptor is homologous to cellular EGF and, therefore, binds to the ErbB family of receptors.19 The signaling through these tyrosine kinase receptors results in DNA synthesis and cell proliferation, including thymidine kinase-induced nucleotide production, thereby increasing vaccinia replication.20 As pancreatic cancers frequently overexpress EGFR, this tumor type represents a promising model for targeted oncolytic vaccinia therapy.21
Pancreatic tumors are often well vascularized and high microvessel density has been shown to correlate with poor prognosis after curative resection.22 Therefore, inhibition of angiogenesis is a rational target for the treatment of pancreatic cancer and many angiogenesis inhibitors have been investigated in animal models of pancreatic cancer,23 resulting in recent clinical trials.24, 25 Despite these efforts, efficacy has been limited. Endostatin and angiostatin are the two potent endogenous angiogenesis inhibitors that have displayed antitumor efficacy in various animal models,26, 27, 28, 29 including pancreatic cancer.27, 29 They act synergistically when used in combination, which led to the construction of an endostatin–angiostatin fusion gene.30 This has been successfully delivered by both viral30, 31, 32, 33 and non-viral vectors.34
The combination of an oncolytic vaccinia virus that also expresses the endostatin–angiostatin fusion gene may provide potent, targeted angiogenesis inhibition on a continuous basis in the local tumor environment to slow tumor growth, allowing the virus to spread through and destroy the tumor. We therefore constructed an oncolytic vaccine strain of vaccinia virus expressing a human endostatin–angiostatin fusion gene (VVhEA). In this report, we tested our hypothesis and show that VVhEA is a potential therapeutic agent targeting human pancreatic cancer.
Results
Lister strain of vaccinia virus is more potent than adenovirus and replicates in human pancreatic cancer cell lines insensitive to adenovirus
To show the potential of the Lister vaccine strain of vaccinia virus as a therapeutic agent for human pancreatic cancer, we compared the cytotoxicity of VVLister and Ad5 in a panel of human pancreatic cancer cell lines in vitro (Figure 1a). VVLister displayed a greater potency than Ad5 in all cell lines tested, including cancer cells insensitive to adenovirus, such as PaTu8988s, Suit-2, HS766T and Capan1. To determine whether vaccinia virus-induced cell killing was indicative of replication induction in cancer cells, replication of VVLister was confirmed in PaTu8988s and Suit-2 (Figures 1b and c).
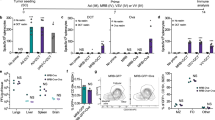
Cytotoxicity and replication of Lister strain of vaccinia virus in human cancer cells and normal epithelial cells. (a) Comparison of cytotoxicity of Lister strain vaccinia virus and adenovirus in a panel of human pancreatic cancer cell lines. Mean EC50 values were derived by MTS assay 6 days after infection of the Lister strain of vaccinia virus and adenovirus, displayed in order of Ad5/VVLister ratio (a value greater than 1.0 indicates that VV Lister was more potent); (b and c) the viral replication of vaccinia virus in human pancreatic cancer cells insensitive to adenovirus; (d) viral replication in human squamous epithelial cells. Cells were infected with 1 PFU per cell (5 PFU per cell for NHEK) of VVLister and cell lysates harvested over a time course. Mean viral replication values±SEM were determined by the TCID50 assay.
Lister vaccine strain of vaccinia virus displays selectivity between tumor cells and normal cells in vitro and in vivo
The Lister strain vaccinia virus has been used for visualization of tumors and metastases and cancer treatment,35, 36, 37 however, the selective resistance of normal human cells was not definitively showed, especially between normal human cells and cancer cells. Therefore, the tumor selectivity in vitro was evaluated by comparing the replication of VVLister in non-immortalized normal and malignant squamous epithelial cell lines. Despite infecting normal human epithelial keratinocytes (NHEKs) cells with five times the dose of VVLister as that used for SCC25 tumor cells, no significant viral replication was seen in NHEK (data not shown) in contrast to the marked viral replication in SCC25 (Figure 1d).
The VVlister vaccinia virus has shown tumor tropism in vivo in mouse models;35, 36, 37, 38 therefore, we investigated whether the virus still has selectivity in our human pancreatic cancer xenograft model by real-time fluorescence imaging and immunohistochemistry (IHC), which confirmed the tumor selectivity of the vaccinia virus in vivo. We first confirmed dose-dependent green fluorescent protein (GFP) expression in Suit-2 cells infected with VVRG in vitro (supplementary Figure 1) before administering BALB/c nude mice bearing Suit-2 xenografts with an i.t. or i.v. injections of VVRG (Figures 2a and b). GFP expression was seen in all tumors after delivery by either route from 24 through to 240 h. Expression after i.t. virus administration increased to a peak at 72 h, whereas after i.v. delivery, levels were still rising 10 days later, suggesting that i.v. delivery of the Lister strain of vaccinia virus may be superior to that of i.t. delivery. Only background activity was observed in tumors of control mice injected with phosphate buffered saline (PBS). Vaccinia virus displayed excellent tumor selectivity with extra-tumoral fluorescence only observed in the tails of three mice after i.v. and one after i.t. deliveries, and the paws of two mice after i.t. delivery, although this resolved by 240 h.
Biodistribution of vaccinia virus in BALB/c nude mice with Suit-2 subcutaneous tumors. (a and b) Biodistribution of VVRG in vivo. Biodistribution of VVRG was ascertained by IVIS imaging under inhalation anesthesia 24, 48, 72, 120 and 240 h after virus administration. Representative images are shown at 120 h (left panel) and combined mean efficiency±SEM (right panel). A total of 1 × 106 cells Suit-2 were seeded by subcutaneous injection into the right flank of 10 BALB/c nude mice. When tumors reached 4–5 mm in diameter, in (a) three mice were injected once i.t. with 1 × 107 PFU VVRG and two mice with PBS as controls and in (b) four mice were injected once i.v. with 1 × 107 PFU VVRG and one mouse with PBS as a control; (c) biodistribution of the Lister strain of vaccinia virus after i.v. injection of 1 × 107 PFU VVRG to BALB/c nude mice with Suit-2 tumors by IHC for Lister coat protein in tumors, spleen, brain and ovaries ( × 200).
The tumor selectivity of the parental VVLister was also confirmed by IHC of tumors and organs harvested from nude mice bearing Suit-2 xenografts after single i.v. virus injection (Figure 2c). VVLister was seen in all tumors from 24 to 480 h after delivery. Selectivity over normal tissues was confirmed, as only monocytes in the spleen were positive for VV coat protein in one of three mice at 24 and 72 h and all three mice from 120 to 480 h. Ovaries, brains, liver, kidneys, lungs and adrenal glands were all negative, including PBS-treated controls (not shown).
Construction, potency and replication of a novel vaccinia virus expressing human endostatin–angiostatin fusion protein
To enhance the efficacy of oncolytic vaccinia virus, the endostatin–angiostatin fusion gene was inserted at the Not1 restriction site of the Lister vaccine strain of vaccinia virus (VVhEA, Figure 3a). Another recombinant virus (VVlacZ) was constructed with the marker gene at the same genomic site serving as a control (Figure 3a). The sequences of inserted genes were confirmed by PCR and sequencing (data not shown). The potency and replication of both recombinant viruses in vitro were consistently less than that of the parental VVLister (Figures 3b, c and d). The potency of VVhEA was also less than that of VVlacZ in all cell lines tested, but there was no significant difference in the levels of peak replication between VVhEA and VVlacZ in PaTu8988s or Suit-2 cells (Figures 3c and d).
Potency and replication of recombinant vaccinia viruses armed with human endostatin–angiostatin fusion gene and LacZ gene. (a) VVlacZ and VVhEA constructions by insertion of the lacZ and human endostatin–angiostatin fusion genes, respectively, into the Not1 restriction site of VVLister; (b) potency of VVhEA and VVLacZ in human pancreatic cancer cell lines. EC50 values+SEM calculated by MTS assay 144 h after infection with different vaccinia viruses; (c and d) replication of recombinant viruses in pancreatic cell lines infected with 1 PFU per cell VVlacZ or VVhEA. Mean viral replication±SEM was determined by TCID50 assay.
The endostatin–angiostatin fusion protein is expressed in Suit-2 cells infected with VVhEA and inhibits HUVEC cell tube formation and proliferation in vitro
The expression of the human endostatin–angiostatin fusion gene in Suit-2 cells infected with VVhEA was confirmed by western blotting (Figure 4a). The anti-angiogenic function of the endostatin–angiostatin fusion protein was confirmed by the inhibition of human umbilical vein epithelial cell (HUVEC) tube formation and proliferation (Figures 4b, c and d). HUVEC tube formation was significantly inhibited by supernatant from Suit-2 cells infected with VVhEA when compared with VVlacZ (P<0.001) or mock-infected controls (Figure 4c). The inhibition of HUVEC proliferation was also significantly greater when treated with VVhEA supernatant than either VVlacZ (P<0.0001) or mock-infected controls (Figure 4d).
Expression and angiogenesis inhibition by the human endostatin–angiostatin fusion protein in Suit-2 cells infected with VVhEA in vitro (a) endostatin–angiostatin fusion protein expression in Suit-2 cells. Suit-2 cells were infected with 1 PFU per cell of VVhEA or VVlacZ. Cells and supernatant were harvested 24, 48 and 72 h later. Western blots were performed as described in Materials and methods. All fusion protein bands were between 70 and 80 kDa and β-actin around 45 kDa. Although intracellular transgene expression was found in the cells by 24 h after infection, endostatin–angiostatin fusion protein was detected in the supernatant only after 48 h; (b and c) inhibition of HUVEC tube formation. HUVEC were seeded in a 96-well BD Biocoat angiogenesis plate containing Matrigel (BD Bioscience, Bedford, MA, USA) with 10 μg of supernatant harvested and concentrated 72 h after Suit-2 cells were infected with 1 PFU per cell of VVhEA or VVlacZ. At 16 h later, 400 μg Calcein AM (Invitrogen, Eugene, OR, USA) was added and fluorescence microscopy used to assess the number of fully formed HUVEC tubes, which were compared with mock-infected controls and each other by one-way ANOVA; (d) inhibition of HUVEC proliferation, mean cell survival±SEM as a percentage of uninfected HUVEC by MTS assay 96 h post-treatment with 10 μg ml−1 of supernatant harvested from Suit-2 cells infected with 1 PFU per cell of VVhEA or VVlacZ for 72 h. Mean results were compared by one-way ANOVA with Bonferonni's post hoc testing.
The endostatin–angiostatin fusion protein is expressed and inhibits angiogenesis in Suit-2 xenografts treated with VVhEA in vivo
The distribution of VVhEA and VVlacZ and human endostatin–angiostatin fusion protein expression were confirmed by IHC in Suit-2 tumors harvested from nude mice after i.v. or i.t. virus injections. The expression of human endostatin–angiostatin in animals after i.t. (Figure 5a) and i.v. (not shown, similar to i.t.) therapies was confirmed from 48 h onwards, with high-intensity immunoreactivity correlated with Lister coat protein staining in spatially similar areas in serial sections. PBS-treated tumors were negative for both proteins (not shown). Fusion protein expression was also confirmed in plasma after i.v. (Figure 5b) and i.t. deliveries (supplementary Figure 2). The level of endostatin expression in plasma after i.v. injection of VVhEA was significantly higher and lasted longer than those after i.t. injection of VVhEA, consistent with the result of reporter gene expression in tumor tissues (Figures 2a and b). The microvessel density in tumors from VVhEA-treated mice was significantly lower than those from VVlacZ-treated mice from 120 h onwards after i.t. treatment (Figure 5c) and 72 h onwards after i.v. delivery (Figure 5d), indicating the inhibition of angiogenesis by the fusion protein.
Expression and angiogenesis inhibition by the human endostatin–angiostatin fusion protein after treatment of Suit-2 tumor model in vivo. (a) IHC for Lister vaccinia virus coat protein and human endostatin was performed on Suit-2 tumors; (b) ELISA for human endostatin performed on plasma harvested from animals after 1 × 107 PFU i.v. VVhEA or VVlacZ with representative images at 48 and 480 h ( × 200); (c and d) IHC for murine CD31 to assess mean microvessel density±SEM in five random × 200 fields of i.t. (c) or i.v. (d) VVhEA-, VVlacZ- or PBS-treated tumors compared by t-tests.
VVhEA prolongs survival of nude mice bearing Suit-2 tumor xenografts after i.t. delivery
The Suit-2 xenograft human pancreatic cancer model was established in BALB/c nude mice and treated with i.t. injections of vaccinia viruses to assess the antitumor potency of the novel vaccinia virus in vivo (Figure 6). Tumors regressed in three of five mice treated with low-dose (three doses at 1 × 107 plaque-forming unit (PFU), Figure 6a) VVhEA therapy, which resulted in significantly longer survival than mice in other groups (Figure 6b). Two of these mice remained alive at the end of the experiment, that is, 91 days after treatment.
Antitumoral efficacy of different vaccinia viruses in established Suit-2 tumors in vivo. Suit-2 human pancreatic carcinoma xenografts implanted subcutaneously in BALB/c nu/nu mice as described in Materials and methods. (a and b) PBS or 1 × 107 PFU of different viruses were injected on days 0, 2 and 4 (n=5 per group); (c and d) 5 × 107 PFU of different viruses and PBS were injected on days 0, 3, 6, 9, 12 and 15 (n=8 per group); (a and c) show the tumor growth curves (until death or killed because of tumor ulceration or weight loss of first animal in each group); (b and d) show the survival rate of nude mice by Kaplan–Meier survival analysis (log-rank test for statistical significance).
High-dose (six doses of 5 × 107 PFU) therapy with all vaccinia viruses resulted in significantly slower rates of tumor growth than in PBS-treated controls (Figure 6c). However, VVLister-treated mice survived for a significantly shorter period as all mice had to be killed as a result of weight loss and sickness by 18 days after their first treatment. Post-mortem analysis found pock lesions on their feet, tails and oral cavities. Mice treated with VVhEA or VVlacZ did not suffer from the same severity of systemic side effects and survived longer than controls (Figure 6d). The VVhEA-treated mice survived significantly longer compared with the VVLacZ-treated mice, although the rate of tumor growth was no different between two groups.
In terms of clinical application, i.v. injection may be more feasible than i.t injection. Therefore, 1 × 107 PFU of VvhEA and VVLacZ were injected intravenously into the Suit-2 bearing nude mice. Unfortunately, all animals treated with recombinant vaccinia viruses developed tumor ulceration and pock lesions on their tails, and had to be sacrificed before showing efficacy.
Discussion
In this study, we first showed that the Lister vaccine strain of vaccinia virus was more potent at tumor cell killing than Ad5 in all cell lines tested, supporting our hypothesis that vaccinia virus represents a promising alternative to adenovirus for cancer gene therapy. The WR strain of vaccinia virus has been used most commonly for the construction of oncolytic vaccinia viruses, based on its superior lytic activity in vitro.17 However, it is a laboratory-based strain, without the advantage of clinical experience as a vaccine. The Lister vaccine strain is an attractive oncolytic virus as its good safety profile has already been proved in humans during the vaccination program against smallpox in Europe and Asia. The recent complete sequencing of the Lister strain of vaccinia virus facilitated its further development and construction of more advanced vectors for gene therapy.39
In addition to its wide tissue tropism, oncolytic vaccinia virus must display tumor selectivity. The Lister vaccine strain does not cause any known human disease.23 However, 80 per million vaccinia vaccinations produced lysis of skin epithelial cells, especially in immunosuppressed individuals, resulting in spreading tissue necrosis known as vaccinia necrosum.40, 41 Therefore, we selected normal squamous cells NHEK (more likely than other tissue origin to support vaccinia virus replication) and compared VVLister replication with SCC25, a human tumor cell line also of squamous cell origin. Only SCC25 supported the replication of vaccinia virus, confirming the selectivity of the Lister stain in vitro.
In a human pancreatic cancer model, we have also showed that the Lister vaccinia virus is inherently tumor-selective after delivery in vivo, evidenced by live fluorescence imaging of VVRG and the biodistribution of i.v. VVLister by IHC. This selectivity was also shown in murine tumor xenograft models (Tysome et al. unpublished data). The Lister vaccine strain vaccinia virus presents a superior safety profile in vivo as the Lister strain, in contrast to the WR strain,9, 18 has not been detected in the ovaries or brains of mice. Most surprisingly, we, for the first time, showed that i.v. delivery of the Lister strain vaccinia virus might be superior to i.t. delivery. This finding may have important implications for the future use of oncolytic vaccinia virus as i.v. therapy could target not only primary tumors, but also metastases. This observation may be strain-dependent, as tumor-specific transgene expression by a TK-deleted WR strain of vaccinia virus expressing cytosine deaminase7 and a Wyeth strain virus expressing GM-CSF (granulocyte-macrophage colony-stimulating factor),42 did not show this feature. Unfortunately, tumor specificity after i.v. delivery in our study did not translate into antitumor efficacy using the standard dose of 1 × 107 PFU, as the routine dose used for oncolytic vaccinia virus in this study was limited by tumor ulceration and pock lesions on the tail, paws and in oral cavities of the nude mice. These side effects may result from the huge viral replication in the ‘factory’ of tumor cells as we have observed that reporter gene and endostatin–angiostatin expressions were significantly higher after i.v. injection than i.t. injection (Figures 2b and 5b). Further, experiments are needed to achieve the optimal regime. In addition, although pock lesions have been reported after vaccinia virus administration to nude mice,43, 44, 45 they have not been observed in immunocompetent mice.44, 45, 46, 47 Therefore, further studies are needed to clarify our findings using immunocompetent tumor models, where the potential for systemic treatment may not be hampered by systemic side effects.
Anti-angiogenic agents, which target activated endothelial cells, represent a promising strategy for the treatment of tumors. However, their development has been hampered by several factors including manufacturing difficulties, stability and solubility issues.48 In addition, the majority of these inhibitors of angiogenesis are not directly cytotoxic to tumor cells so they need to be expressed on a continuous basis. Given the tumor-specific replication of oncolytic vaccinia virus, it is timely to explore their use to engineer inhibition of angiogenesis. We constructed a novel oncolytic Lister strain of vaccinia virus armed with a human endostatin–angiostatin fusion gene targeting the process of neovascularisation. The continuous expression and angiogenesis inhibition of the endostatin–angiostatin fusion protein was confirmed in the Suit-2 pancreatic cancer model both in vitro and up to 20 days after one treatment in vivo. We found that the potency and replication of both F14.5L-deleted viruses (VVhEA and VvlacZ) were attenuated when compared with the parental VVLister virus. We anticipate that this was because of insertional inactivation at the NotI site of the hypothetical protein F3 encoded by a small gene located between F14L (List049) and F15L (List050) of the genome.39 The vaccinia F3 protein may be involved in immune evasion, accounting for viral attenuation after deletion. This concept was recently confirmed by others using VVRG (described by the authors as GLV-ld27).38
The VVhEA therapy resulted in significantly longer survival when compared with VVlacZ-treated mice in vivo, with regression in three of five tumors after low dose, and all tumors after high-dose therapy. However, tumor regression was also seen after high-dose treatment of all vaccinia viruses, although survival was only prolonged with VVhEA and VVlacZ, when compared with PBS. The attenuation of both recombinant viruses resulted in fewer side effects in immunodeficient mice in vivo, as VVLister-treated mice developed more pock lesions and rapidly lost weight, requiring their sacrifice even before PBS-treated controls. The survival advantage of VVhEA over VVlacZ after high-dose therapy may have been because of the VVhEA-mediated inhibition of angiogenesis affecting i.t. propagation of the virus and thus spread and distribution of the virus throughout the mice, which may have reduced the side effect. In addition, VVhEA may reverse VEGF-induced cancer-associated systemic syndrome and prevent death in tumor-bearing mice without significantly compromising tumor growth.49 Although the added benefit of the fusion gene in VVhEA over VVlacZ was not as great as might have been expected, these results obviously warrant further investigation in an immunocompetent model as anti-angiogenesis therapy can overcome endothelial cell anergy, promote leukocyte-endothelium interactions and inhibit tumor growth and microvessel density significantly, with remarked infiltration of leukocytes (CD45), as well as the number of CD8+ cytotoxic T lymphocytes in tumors.50
In conclusion, we show the superior antitumor potency of the Lister strain of vaccinia virus over wild-type adenovirus against pancreatic cancer, especially for tumor cell lines insensitive to adenovirus. The virus also displays inherently high selectivity for cancer cells, sparing normal cells both in vitro and in vivo. Through arming the Lister strain with the human endostatin–angiostatin fusion gene, we combined the anti-angiogenic properties of the fusion protein with the oncolytic properties of the Lister virus. This novel recombinant virus has shown efficacy in terms of tumor regression and prolonged survival in a human pancreatic cancer xenograft model and shows potential for translation to clinical therapy in the future.
Materials and methods
Cell lines
CV1, the African Green Monkey normal kidney cell line was obtained from the American Type Culture Collection (ATCC, Manassas, VA, USA) and cultured in DMEM (Dulbecco's Modified Eagle's Medium) supplemented with 10% fetal calf serum (FCS). HUVECs and NHEKs were obtained from Cambrex (Cambridge, UK) and maintained in epithelial growth medium-2 (EGM-2) and keratinocyte growth medium (KGM), respectively.
Human pancreatic carcinoma cell lines Suit-2, PaTu8988S, PaTu8988T, MiaPaCa2, PANC1 and Capan1 were maintained in DMEM with 10% FCS. The human HNSCC cell line, SCC25, was obtained from Cancer Research UK Cell Culture Service (CRUKCCS) and maintained in DMEM:HAMSF12 in the ratio of 1:1 with 10% FCS and 400 ng ml−1 hydrocortisone (Sigma-Aldrich, St Louis, MO, USA).
Viruses
The Lister vaccine strain (LIVP) of vaccinia virus was used as a parental virus for the construction of recombinant viruses.43 The fused human endostatin and angiostatin genes were inserted following the method described earlier51 into the non-essential NotI restriction site, located between F14L and F15L of the LIVP and encoding a hypothetical protein, F3. VVlacZ was constructed in the same way after insertion of the E. coli lacZ gene, to serve as a control for VVhEA. PCR and DNA sequencing were used to verify recombinant viruses. In an earlier study, the Renilla luciferase-GFP fusion gene was inserted into the same region to create VVRG.43 Wild-type adenovirus Ad5 was described earlier.52
Evaluation of viral cytotoxicity in vitro
Cells were seeded at 1 and 5 × 103 cells per well, depending on growth rates, in 96-well plates, and infected with viruses 16–18 h later. Cell survival on day 6 after viral infection was determined by MTS (3-(4,5-dimethylthiazol-2-yl)-5-(3-carboxymethoxyphenyl)-2-(4-sulfophenyl)-2H-tetrazolium) assay and EC50 value (viral dose killing 50% of tumor cells) was calculated as described earlier.52 All assays were performed at least three times.
Viral replication
Cells were seeded at 2–4 × 105 cells per well, depending on growth rates, in three wells of 6-well plates in media with 10% FCS, and infected with 1 PFU per cell of vaccinia viruses 16–18 h later. Samples were harvested in triplicate at 24-h intervals up to 144 h. Viral replication was detected by TCID50 (50% tissue culture infective dose) as described earlier.52
Biodistribution of VVRG by fluorescence imaging in vivo
A total of 1 × 106 Suit-2 cells were implanted subcutaneously into the right flank of 10 female BALB/c nude mice (Harlan UK Ltd, Bicester, UK). When tumors reached 0.4–0.5 cm in diameter, mice received 100 μl i.t. or i.v. tail vein injections of 1.0 × 108 PFU VVRG or PBS. The biodistribution of VVRG was determined in mice anesthetized (2% halothane by inhalation in O2 1 l min−1 and NO 1 l min−1) 1, 2, 3, 5 and 10 days after treatment by measuring fluorescence with the IVIS camera (Xenogen Corp., Alameda, CA, USA) in tumors defined as region of interest (ROI) after imaging. All animal experiments were performed in accordance with the regulations of the UK Home Office and the local animal ethics committee.
Western blotting
A total of 2 × 105 Suit-2 cells were seeded in 60 mm dishes in conditional media and infected with 1 PFU per cell VVhEA or VVlacZ in DMEM with 2% FCS after 16–18 h. Cells and supernatant were harvested separately 24, 48 and 72 h after infection and supernatants concentrated using Centricon 10 kDa columns (Millipore, Bedford, MA, USA). A total of 30 μg aliquots of total protein were used to detect endostatin–angiostatin fusion protein expression by western blotting as described earlier.53
HUVEC proliferation and tube formation assay
A total of 1 × 104 HUVEC cells were seeded in 96-well plates in EGM-2 and treated 16–18 h later with 10 μg ml−1 of supernatant concentrated from Suit-2 cells infected with VVlacZ or VVhEA for 72 h. After another 96 h, cell viability was measured by MTS assay to determine HUVEC proliferation.
The inhibition of HUVEC tube formation was observed using the BD Biocoat angiogenesis system (BD Biosciences, Bedford, MA, USA) according to the manufacturer's instructions. Tube formation by HUVEC treated with supernatant was compared with mock-infected HUVEC alone by counting the number of completely formed tubes/well by fluorescence microscopy.
Histopathology and immunohistochemistry staining
When established Suit-2 tumors reached 0.4–0.5 cm in diameter, mice were stratified into groups of 18. Each received one 100-μl i.v. or i.t. injection of 1.0 × 107 PFU of VVLister, VVhEA, VVlacZ or PBS. Groups of three mice in each cohort were killed 24, 48, 72, 120, 240 and 480 h later, tumors removed, snap-frozen in isopentane and stored at −80 °C. Blood was collected into a heparinized tube and plasma stored at −80 °C. From animals that had received i.v. VVLister or PBS, the spleen, liver, kidneys, brain, ovaries, lungs and adrenal glands were also collected and stored. All tissues were processed for histopathology and IHC analyses for viral coat protein (1:2000 rabbit anti-vaccinia virus coat protein polyclonal antibody (MorphoSys UK Ltd, Bath, UK)), endostatin expression (1:250 rabbit anti-human endostatin polyclonal antibody (Abcam, Cambridge, UK)) and CD31 (1:200 rat anti-murine CD31 antibody (BD Biosciences, Oxford, UK)) to determine microvessel density as described earlier.54
ELISA
Human endostatin levels in the plasma of BALB/c nu/nu mice bearing Suit-2 xenografts treated with i.v. VVhEA, VVlacZ or PBS were obtained using the Duoset ELISA for human endostatin (R and D Systems, Abingdon, UK unless otherwise stated) according to the manufacturers' instructions.
In vivo efficacy experiments
As described above, when established Suit-2 xenografts of 20 mice reached 0.4–0.5 cm in diameter, mice were regrouped by tumor size and received 100 μl i.t. injections of 1.0 × 107 PFU VVLister, VVlacZ, VVhEA or PBS on days 0, 2 and 4. Tumor volumes were estimated (volume=(length × width2 × π)/6) twice weekly until mice were killed when tumor volume reached 1.00 cm3 or had been present for 3 months. This was repeated in experiments, in which 36 mice with Suit-2 xenografts received 5.0 × 107 PFU i.t. injections on days 0, 3, 6, 9, 12 and 15, and 20 mice with Suit-2 xenografts received 1.0 × 107 PFU i.v. injection on day 0, when tumor xenografts reached 0.8–0.5 cm.
Statistical analysis
All statistical analyses were performed as described in figure legends or results. Differences were considered significant where P<0.05.
Conflict of interest
The authors declare no conflict of interest.
References
Hezel AF, Kimmelman AC, Stanger BZ, Bardeesy N, Depinho RA . Genetics and biology of pancreatic ductal adenocarcinoma. Genes Dev 2006; 20: 1218–1249.
Kleeff J, Michalski C, Friess H, Buchler MW . Pancreatic cancer: from bench to 5-year survival. Pancreas 2006; 33: 111–118.
Bhattacharyya M, Lemoine NR . Gene therapy developments for pancreatic cancer. Best Pract Res Clin Gastroenterol 2006; 20: 285–298.
Garber K . China approves world's first oncolytic virus therapy for cancer treatment. J Natl Cancer Inst 2006; 98: 298–300.
Hecht JR, Bedford R, Abbruzzese JL, Lahoti S, Reid TR, Soetikno RM et al. A phase I/II trial of intratumoral endoscopic ultrasound injection of ONYX-015 with intravenous gemcitabine in unresectable pancreatic carcinoma. Clin Cancer Res 2003; 9: 555–561.
Rein DT, Breidenbach M, Curiel DT . Current developments in adenovirus-based cancer gene therapy. Future Oncol 2006; 2: 137–143.
Gnant MF, Puhlmann M, Alexander Jr HR, Bartlett DL . Systemic administration of a recombinant vaccinia virus expressing the cytosine deaminase gene and subsequent treatment with 5-fluorocytosine leads to tumor-specific gene expression and prolongation of survival in mice. Cancer Res 1999; 59: 3396–3403.
Hung CF, Tsai YC, He L, Coukos G, Fodor I, Qin L et al. Vaccinia virus preferentially infects and controls human and murine ovarian tumors in mice. Gene Therapy 2007; 14: 20–29.
McCart JA, Ward JM, Lee J, Hu Y, Alexander HR, Libutti SK et al. Systemic cancer therapy with a tumor-selective vaccinia virus mutant lacking thymidine kinase and vaccinia growth factor genes. Cancer Res 2001; 61: 8751–8757.
Puhlmann M, Brown CK, Gnant M, Huang J, Libutti SK, Alexander HR et al. Vaccinia as a vector for tumor-directed gene therapy: biodistribution of a thymidine kinase-deleted mutant. Cancer Gene Ther 2000; 7: 66–73.
Thorne SH, Bartlett DL, Kirn DH . The use of oncolytic vaccinia viruses in the treatment of cancer: a new role for an old ally? Curr Gene Ther 2005; 5: 429–443.
Slobod KS, Lockey TD, Howlett N, Srinivas RV, Rencher SD, Freiden PJ et al. Subcutaneous administration of a recombinant vaccinia virus vaccine expressing multiple envelopes of HIV-1. Eur J Clin Microbiol Infect Dis 2004; 23: 106–110.
Rochlitz C, Figlin R, Squiban P, Salzberg M, Pless M, Herrmann R et al. Phase I immunotherapy with a modified vaccinia virus (MVA) expressing human MUC1 as antigen-specific immunotherapy in patients with MUC1-positive advanced cancer. J Gene Med 2003; 5: 690–699.
Mastrangelo MJ, Maguire Jr HC, Eisenlohr LC, Laughlin CE, Monken CE, McCue PA et al. Intratumoral recombinant GM-CSF-encoding virus as gene therapy in patients with cutaneous melanoma. Cancer Gene Ther 1999; 6: 409–422.
Gomella LG, Mastrangelo MJ, McCue PA, Maguire HJ, Mulholland SG, Lattime EC . Phase I study of intravesical vaccinia virus as a vector for gene therapy of bladder cancer. J Urol 2001; 166: 1291–1295.
Alemany R . A smart move against cancer for vaccinia virus. Lancet Oncol 2008; 9: 507–508.
Guo ZS, Bartlett DL . Vaccinia as a vector for gene delivery. Expert Opin Biol Ther 2004; 4: 901–917.
Luker KE, Hutchens M, Schultz T, Pekosz A, Luker GD . Bioluminescence imaging of vaccinia virus: effects of interferon on viral replication and spread. Virology 2005; 341: 284–300.
Stein RA, Staros JV . Evolutionary analysis of the ErbB receptor and ligand families. J Mol Evol 2000; 50: 397–412.
Tzahar E, Moyer JD, Waterman H, Barbacci EG, Bao J, Levkowitz G et al. Pathogenic poxviruses reveal viral strategies to exploit the ErbB signaling network. EMBO J 1998; 17: 5948–5963.
Lemoine NR, Hughes CM, Barton CM, Poulsom R, Jeffery RE, Kloppel G et al. The epidermal growth factor receptor in human pancreatic cancer. J Pathol 1992; 166: 7–12.
Ikeda N, Adachi M, Taki T, Huang C, Hashida H, Takabayashi A et al. Prognostic significance of angiogenesis in human pancreatic cancer. Br J Cancer 1999; 79: 1553–1563.
Garcea G, Doucas H, Steward WP, Dennison AR, Berry DP . Hypoxia and angiogenesis in pancreatic cancer. ANZ J Surg 2006; 76: 830–842.
Ferrari V, Valcamonico F, Amoroso V, Simoncini E, Vassalli L, Marpicati P et al. Gemcitabine plus celecoxib (GECO) in advanced pancreatic cancer: a phase II trial. Cancer Chemother Pharmacol 2006; 57: 185–190.
Friess H, Langrehr JM, Oettle H, Raedle J, Niedergethmann M, Dittrich C et al. A randomized multi-center phase II trial of the angiogenesis inhibitor Cilengitide (EMD 121974) and gemcitabine compared with gemcitabine alone in advanced unresectable pancreatic cancer. BMC Cancer 2006; 6: 285.
Hebert C, Siavash H, Norris K, Nikitakis NG, Sauk JJ . Endostatin inhibits nitric oxide and diminishes VEGF and collagen XVIII in squamous carcinoma cells. Int J Cancer 2005; 114: 195–201.
Nie SL, Yuan SZ . Experimental study of gene therapy with angiostatin gene in pancreatic cancer. Hepatobiliary Pancreat Dis Int 2002; 1: 452–457.
Schmitz V, Wang L, Barajas M, Gomar C, Prieto J, Qian C . Treatment of colorectal and hepatocellular carcinomas by adenoviral mediated gene transfer of endostatin and angiostatin-like molecule in mice. Gut 2004; 53: 561–567.
Zhang X, Xu J, Lawler J, Terwilliger E, Parangi S . Adeno-associated virus-mediated antiangiogenic gene therapy with thrombospondin-1 type 1 repeats and endostatin. Clin Cancer Res 2007; 13: 3968–3976.
Scappaticci FA, Contreras A, Smith R, Bonhoure L, Lum B, Cao Y et al. Statin-AE: a novel angiostatin–endostatin fusion protein with enhanced antiangiogenic and antitumor activity. Angiogenesis 2001; 4: 263–268.
Li X, Liu YH, Lee SJ, Gardner TA, Jeng MH, Kao C . Prostate-restricted replicative adenovirus expressing human endostatin–angiostatin fusion gene exhibiting dramatic antitumor efficacy. Clin Cancer Res 2008; 14: 291–299.
Raikwar SP, Temm CJ, Raikwar NS, Kao C, Molitoris BA, Gardner TA . Adenoviral vectors expressing human endostatin–angiostatin and soluble Tie2: enhanced suppression of tumor growth and antiangiogenic effects in a prostate tumor model. Mol Ther 2005; 12: 1091–1100.
Yang CT, Lin YC, Lin CL, Lu J, Bu X, Tsai YH et al. Oncolytic herpesvirus with secretable angiostatic proteins in the treatment of human lung cancer cells. Anticancer Res 2005; 25: 2049–2054.
Weiss JM, Shivakumar R, Feller S, Li LH, Hanson A, Fogler WE et al. Rapid, in vivo, evaluation of antiangiogenic and antineoplastic gene products by nonviral transfection of tumor cells. Cancer Gene Ther 2004; 11: 346–353.
Fodor I, Timiryasova T, Denes B, Yoshida J, Ruckle H, Lilly M . Vaccinia virus mediated p53 gene therapy for bladder cancer in an orthotopic murine model. J Urol 2005; 173: 604–609.
Kelly KJ, Woo Y, Brader P, Yu Z, Riedl C, Lin SF et al. Novel oncolytic agent GLV-1h68 is effective against malignant pleural mesothelioma. Hum Gene Ther 2008; 19: 774–782.
Yu YA, Shabahang S, Timiryasova TM, Zhang Q, Beltz R, Gentschev I et al. Visualization of tumors and metastases in live animals with bacteria and vaccinia virus encoding light-emitting proteins. Nat Biotechnol 2004; 22: 313–320.
Zhang Q, Yu YA, Wang E, Chen N, Danner RL, Munson PJ et al. Eradication of solid human breast tumors in nude mice with an intravenously injected light-emitting oncolytic vaccinia virus. Cancer Res 2007; 67: 10038–10046.
Garcel A, Crance JM, Drillien R, Garin D, Favier AL . Genomic sequence of a clonal isolate of the vaccinia virus Lister strain employed for smallpox vaccination in France and its comparison to other orthopoxviruses. J Gen Virol 2007; 88: 1906–1916.
Gurvich EB, Gomes LA, Yartsev MN, Khakhalin LN, Grigor'eva LB, Dmitrieva NG et al. Vaccinia virus persistence in a child against the background of immune deficiency. J Hyg Epidemiol Microbiol Immunol 1986; 30: 177–183.
Poland GA, Grabenstein JD, Neff JM . The US smallpox vaccination program: a review of a large modern era smallpox vaccination implementation program. Vaccine 2005; 23: 2078–2081.
Kim JH, Oh JY, Park BH, Lee DE, Kim JS, Park HE et al. Systemic armed oncolytic and immunologic therapy for cancer with JX-594, a targeted poxvirus expressing GM-CSF. Mol Ther 2006; 14: 361–370.
Denes B, Gridley DS, Fodor N, Takatsy Z, Timiryasova TM, Fodor I . Attenuation of a vaccine strain of vaccinia virus via inactivation of interferon viroceptor. J Gene Med 2006; 8: 814–823.
Hutt LM . The immune response to infection with vaccinia virus in mice. I. Infection and the production of antibody neutralizing cell-associated and cell-free virus. J Hyg (Lond) 1975; 74: 301–314.
Ober BT, Bruhl P, Schmidt M, Wieser V, Gritschenberger W, Coulibaly S et al. Immunogenicity and safety of defective vaccinia virus lister: comparison with modified vaccinia virus Ankara. J Virol 2002; 76: 7713–7723.
Kirn DH, Wang Y, Le Boeuf F, Bell J, Thorne SH . Targeting of interferon-beta to produce a specific, multi-mechanistic oncolytic vaccinia virus. PLoS Med 2007; 4: e353.
Thorne SH, Hwang TH, O'Gorman WE, Bartlett DL, Sei S, Kanji F et al. Rational strain selection and engineering creates a broad-spectrum, systemically effective oncolytic poxvirus, JX-963. J Clin Invest 2007; 117: 3350–3358.
Hermiston TW, Kuhn I . Armed therapeutic viruses: strategies and challenges to arming oncolytic viruses with therapeutic genes. Cancer Gene Ther 2002; 9: 1022–1035.
Xue Y, Religa P, Cao R, Hansen AJ, Lucchini F, Jones B et al. Anti-VEGF agents confer survival advantages to tumor-bearing mice by improving cancer-associated systemic syndrome. Proc Natl Acad Sci USA 2008; 105: 18513–18518.
Dirkx AE, oude Egbrink MG, Castermans K, van der Schaft DW, Thijssen VL, Dings RP et al. Anti-angiogenesis therapy can overcome endothelial cell anergy and promote leukocyte-endothelium interactions and infiltration in tumors. FASEB J 2006; 20: 621–630.
Timiryasova TM, Chen B, Fodor N, Fodor I . Construction of recombinant vaccinia viruses using PUV-inactivated virus as a helper. Biotechniques 2001; 31: 534–536, 538, 540.
Wang Y, Hallden G, Hill R, Anand A, Liu TC, Francis J et al. E3 gene manipulations affect oncolytic adenovirus activity in immunocompetent tumor models. Nat Biotechnol 2003; 21: 1328–1335.
Wang Y, Xue SA, Hallden G, Francis J, Yuan M, Griffin BE et al. Virus-associated RNA I-deleted adenovirus, a potential oncolytic agent targeting EBV-associated tumors. Cancer Res 2005; 65: 1523–1531.
Kaufman HL, Deraffele G, Mitcham J, Moroziewicz D, Cohen SM, Hurst-Wicker KS et al. Targeting the local tumor microenvironment with vaccinia virus expressing B7.1 for the treatment of melanoma. J Clin Invest 2005; 115: 1903–1912.
Acknowledgements
This project is supported by Cancer Research UK (C633-A6253/A6251), Nature Sciences Foundation of China (30530800) and The Royal College of Surgeons of England (JT) and Barts and The London Research Advisory Board. IF was sponsored by the US Army/National Medical Technology Testbed Inc. We appreciate the critical and insightful comments from Dr Gunnel Hallden. We are grateful to Mr John Overton for his pilot experiments in vitro. We also appreciate Vipul Bhakta, Keyur Trivedi and Mohamed Ikram for IHC staining.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Supplementary Information accompanies the paper on Gene Therapy website (http://www.nature.com/gt)
Supplementary information
Rights and permissions
About this article
Cite this article
Tysome, J., Briat, A., Alusi, G. et al. Lister strain of vaccinia virus armed with endostatin–angiostatin fusion gene as a novel therapeutic agent for human pancreatic cancer. Gene Ther 16, 1223–1233 (2009). https://doi.org/10.1038/gt.2009.74
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gt.2009.74
Keywords
This article is cited by
-
Novel oncolytic chimeric orthopoxvirus causes regression of pancreatic cancer xenografts and exhibits abscopal effect at a single low dose
Journal of Translational Medicine (2018)
-
Lister strain vaccinia virus with thymidine kinase gene deletion is a tractable platform for development of a new generation of oncolytic virus
Gene Therapy (2015)
-
A marker-free system for highly efficient construction of vaccinia virus vectors using CRISPR Cas9
Molecular Therapy - Methods & Clinical Development (2015)
-
Treatment of medulloblastoma with oncolytic measles viruses expressing the angiogenesis inhibitors endostatin and angiostatin
BMC Cancer (2014)
-
Molecular imaging of oncolytic viral therapy
Molecular Therapy - Oncolytics (2014)