Abstract
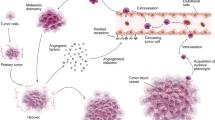
Antiangiogenic cancer therapy is based on agents that target blood vessels of the tumor to inhibit its growth. However, experience from the clinic demonstrates that survival benefits following antiangiogenic therapy do not always correlate with tumor size and growth inhibition. Emerging evidence shows that delivery of antiangiogenic drugs might induce systemic alterations of the vasculature that modulate the function of various tissues and organs. Normalization of tissues and organs by antiangiogenic therapy may be an important mechanism underlying the survival benefits seen in patients with cancer who suffer cancer-associated systemic syndromes. This new concept has been validated in preclinical tumor models, and responses in patients have positively correlated with clinical benefits.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Cao, Y. & Langer, R. Optimizing the delivery of cancer drugs that block angiogenesis. Sci. Transl. Med. 2, 15ps13 (2010).
Kerbel, R. S. Improving conventional or low dose metronomic chemotherapy with targeted antiangiogenic drugs. Cancer Res. Treat. 39, 150–159 (2007).
Hurwitz, H. et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N. Engl. J. Med. 350, 2335–2342 (2004).
Motzer, R. J. et al. Sunitinib versus interferon alfa in metastatic renal-cell carcinoma. N. Engl. J. Med. 356, 115–124 (2007).
Kornguth, S. E. Neuronal proteins and paraneoplastic syndromes. N. Engl. J. Med. 321, 1607–1608 (1989).
Tisdale, M. J. Cachexia in cancer patients. Nat. Rev. Cancer 2, 862–871 (2002).
Escudier, B. et al. Sorafenib in advanced clear-cell renal-cell carcinoma. N. Engl. J. Med. 356, 125–134 (2007).
Azizi, M., Chedid, A. & Oudard, S. Home blood-pressure monitoring in patients receiving sunitinib. N. Engl. J. Med. 358, 95–97 (2008).
Ebos, J. M., Lee, C. R., Christensen, J. G., Mutsaers, A. J. & Kerbel, R. S. Multiple circulating proangiogenic factors induced by sunitinib malate are tumor-independent and correlate with antitumor efficacy. Proc. Natl Acad. Sci. USA 104, 17069–17074 (2007).
Kamba, T. et al. VEGF-dependent plasticity of fenestrated capillaries in the normal adult microvasculature. Am. J. Physiol. Heart Circ. Physiol. 290, H560–H576 (2006).
Xue, Y. et al. Anti-VEGF agents confer survival advantages to tumor-bearing mice by improving cancer-associated systemic syndrome. Proc. Natl Acad. Sci. USA 105, 18513–18518 (2008).
Wong, A. K. et al. Excessive tumor-elaborated VEGF and its neutralization define a lethal paraneoplastic syndrome. Proc. Natl Acad. Sci. USA 98, 7481–7486 (2001).
Cao, Y., Zhong, W. & Sun, Y. Improvement of antiangiogenic cancer therapy by understanding the mechanisms of angiogenic factor interplay and drug resistance. Semin. Cancer Biol. 19, 338–343 (2009).
Harper, S. J. & Bates, D. O. VEGF-A splicing: the key to anti-angiogenic therapeutics? Nat. Rev. Cancer 8, 880–887 (2008).
Neufeld, G., Cohen, T., Gengrinovitch, S. & Poltorak, Z. Vascular endothelial growth factor (VEGF) and its receptors. FASEB J. 13, 9–22 (1999).
Longo, R. & Gasparini, G. Challenges for patient selection with VEGF inhibitors. Cancer Chemother. Pharmacol. 60, 151–170 (2007).
Poon, R. T., Fan, S. T. & Wong, J. Clinical implications of circulating angiogenic factors in cancer patients. J. Clin. Oncol. 19, 1207–1225 (2001).
Nguyen, M. et al. Elevated levels of an angiogenic peptide, basic fibroblast growth factor, in the urine of patients with a wide spectrum of cancers. J. Natl Cancer Inst. 86, 356–361 (1994).
Krzystek-Korpacka, M. et al. Impact of weight loss on circulating IL-1, IL-6, IL-8, TNF-alpha, VEGF-A, VEGF-C and midkine in gastroesophageal cancer patients. Clin. Biochem. 40, 1353–1360 (2007).
Ninck, S. et al. Expression profiles of angiogenic growth factors in squamous cell carcinomas of the head and neck. Int. J. Cancer 106, 34–44 (2003).
Hattori, K. et al. Vascular endothelial growth factor and angiopoietin-1 stimulate postnatal hematopoiesis by recruitment of vasculogenic and hematopoietic stem cells. J. Exp. Med. 193, 1005–1014 (2001).
Nakayama, T., Mutsuga, N. & Tosato, G. Effect of fibroblast growth factor 2 on stromal cell-derived factor 1 production by bone marrow stromal cells and hematopoiesis. J. Natl Cancer Inst. 99, 223–235 (2007).
Nathanson, L. & Hall, T. C. Introduction: paraneoplastic syndromes. Semin. Oncol. 24, 265–268 (1997).
Aoyagi, T., Mori, I., Ueyama, Y. & Tamaoki, N. Sinusoidal dilatation of the liver as a paraneoplastic manifestation of renal cell carcinoma. Hum. Pathol. 20, 1193–1197 (1989).
Oya, M. Renal cell carcinoma: biological features and rationale for molecular-targeted therapy. Keio J. Med. 58, 1–11 (2009).
Shinojima, T. et al. Renal cancer cells lacking hypoxia inducible factor (HIF)-1alpha expression maintain vascular endothelial growth factor expression through HIF-2alpha. Carcinogenesis 28, 529–536 (2007).
Makino, Y. et al. Inhibitory PAS domain protein is a negative regulator of hypoxia-inducible gene expression. Nature 414, 550–554 (2001).
Maxwell, P. H. et al. The tumour suppressor protein VHL targets hypoxia-inducible factors for oxygen-dependent proteolysis. Nature 399, 271–275 (1999).
Maranchie, J. K. et al. The contribution of VHL substrate binding and HIF1-alpha to the phenotype of VHL loss in renal cell carcinoma. Cancer Cell 1, 247–255 (2002).
Tenan, M. et al. Thrombospondin-1 is downregulated by anoxia and suppresses tumorigenicity of human glioblastoma cells. J. Exp. Med. 191, 1789–1798 (2000).
O'Reilly, M. S. et al. Angiostatin: a novel angiogenesis inhibitor that mediates the suppression of metastases by a Lewis lung carcinoma. Cell 79, 315–328 (1994).
Theou-Anton, N., Faivre, S., Dreyer, C. & Raymond, E. Benefit-risk assessment of sunitinib in gastrointestinal stromal tumours and renal cancer. Drug Saf. 32, 717–734 (2009).
Dahlberg, S. E., Sandler, A. B., Brahmer, J. R., Schiller, J. H. & Johnson, D. H. Clinical course of advanced non-small-cell lung cancer patients experiencing hypertension during treatment with bevacizumab in combination with carboplatin and paclitaxel on ECOG 4599. J. Clin. Oncol. 28, 949–954 (2010).
van Heeckeren, W. J., Ortiz, J., Cooney, M. M. & Remick, S. C. Hypertension, proteinuria, and antagonism of vascular endothelial growth factor signaling: clinical toxicity, therapeutic target, or novel biomarker? J. Clin. Oncol. 25, 2993–2995 (2007).
Scartozzi, M. et al. Arterial hypertension correlates with clinical outcome in colorectal cancer patients treated with first-line bevacizumab. Ann. Oncol. 20, 227–230 (2009).
Ravaud, A. & Sire, M. Arterial hypertension and clinical benefit of sunitinib, sorafenib and bevacizumab in first and second-line treatment of metastatic renal cell cancer. Ann. Oncol. 20, 966–967 (2009).
Wick, A. et al. Arterial hypertension and bevacizumab treatment in glioblastoma: no correlation with clinical outcome. J. Neurooncol. 97, 157–158 (2010).
Kappers, M. H., van Esch, J. H., Sleijfer, S., Danser, A. H. & van den Meiracker, A. H. Cardiovascular and renal toxicity during angiogenesis inhibition: clinical and mechanistic aspects. J. Hypertens. 27, 2297–2309 (2009).
Schneider, B. P. et al. Association of vascular endothelial growth factor and vascular endothelial growth factor receptor-2 genetic polymorphisms with outcome in a trial of paclitaxel compared with paclitaxel plus bevacizumab in advanced breast cancer: ECOG 2100. J. Clin. Oncol. 26, 4672–4678 (2008).
Desai, J. et al. Hypothyroidism after sunitinib treatment for patients with gastrointestinal stromal tumors. Ann. Intern. Med. 145, 660–664 (2006).
Rini, B. I. et al. Hypothyroidism in patients with metastatic renal cell carcinoma treated with sunitinib. J. Natl Cancer Inst. 99, 81–83 (2007).
Torino, F., Corsello, S. M., Longo, R., Barnabei, A. & Gasparini, G. Hypothyroidism related to tyrosine kinase inhibitors: an emerging toxic effect of targeted therapy. Nat. Rev. Clin. Oncol. 6, 219–228 (2009).
Steeghs, N. et al. Hypertension and rarefaction during treatment with telatinib, a small molecule angiogenesis inhibitor. Clin. Cancer Res. 14, 3470–3476 (2008).
Saif, M. W., Longo, W. L. & Israel, G. Correlation between rash and a positive drug response associated with bevacizumab in a patient with advanced colorectal cancer. Clin. Colorectal Cancer 7, 144–148 (2008).
Vincenzi, B. et al. Early skin toxicity as a predictive factor for tumor control in hepatocellular carcinoma patients treated with sorafenib. Oncologist 15, 85–92 (2010).
Jain, R. K. Normalizing tumor vasculature with anti-angiogenic therapy: a new paradigm for combination therapy. Nat. Med. 7, 987–989 (2001).
Mancuso, M. R. et al. Rapid vascular regrowth in tumors after reversal of VEGF inhibition. J. Clin. Invest. 116, 2610–2621 (2006).
Hedlund, E. M., Hosaka, K., Zhong, Z., Cao, R. & Cao, Y. Malignant cell-derived PlGF promotes normalization and remodeling of the tumor vasculature. Proc. Natl Acad. Sci. USA 106, 17505–17510 (2009).
Ledford, H. Drug markers questioned. Nature 452, 510–511 (2008).
Folkman, J. Tumor angiogenesis: therapeutic implications. N. Engl. J. Med. 285, 1182–1186 (1971).
Foulkes, W. D., Reis-Filho, J. S. & Narod, S. A. Tumor size and survival in breast cancer—a reappraisal. Nat. Rev. Clin. Oncol. 7, 348–353 (2010).
Longo, R. et al. Anti-angiogenic therapy: rationale, challenges and clinical studies. Angiogenesis 5, 237–256 (2002).
Acknowledgements
The author's laboratory is supported by research grants from the Swedish Research Council, the Swedish Cancer Foundation, the Karolinska Institute Foundation, the Karolinska Institute Distinguished Professor Award, the European Union Integrated Project of Metoxia (project number 222741), and the European Research Council (ERC) Advanced Grant ANGIOFAT (project number 250021).
Author information
Authors and Affiliations
Ethics declarations
Competing interests
Y. Cao is on the Board of Directors at Clanotech.
Rights and permissions
About this article
Cite this article
Cao, Y. Off-tumor target—beneficial site for antiangiogenic cancer therapy?. Nat Rev Clin Oncol 7, 604–608 (2010). https://doi.org/10.1038/nrclinonc.2010.118
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrclinonc.2010.118
This article is cited by
-
Nuclear PD-L1 promotes EGR1-mediated angiogenesis and accelerates tumorigenesis
Cell Discovery (2023)
-
Targeting angiogenesis in oncology, ophthalmology and beyond
Nature Reviews Drug Discovery (2023)
-
The 150 most important questions in cancer research and clinical oncology series: questions 76–85
Chinese Journal of Cancer (2017)
-
Future options of anti-angiogenic cancer therapy
Chinese Journal of Cancer (2016)
-
Inhibition of hypoxia-inducible factor via upregulation of von Hippel-Lindau protein induces “angiogenic switch off” in a hepatoma mouse model
Molecular Therapy - Oncolytics (2015)