Abstract
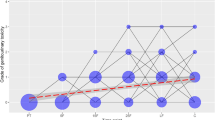
A significant proportion of men undergoing ‘curative’ radical prostatectomy (RP) for organ-confined prostate cancer relapse within 5 years. A number of adverse risk factors have been identified, but to date no adjuvant treatment as improved the outlook for these men. We proposed that these patients, despite small tumour burdens, may be immunosuppressed from their cancer, which may be amenable to immune modulation. We investigated their immune profile using sensitive functional cytokine assays, both pre- and post-surgery. In comparison with controls, RP patients expressed higher levels of both T helper type 1 (Th1) (interleukin (IL)-2 and tumour necrosis factor-α) and Th2 cytokines (IL-4, -5 and -10) with little change after removal of tumour. Further analysis based on known poor-prognostic factors indicated a trend to expression of higher levels of Th2 cytokines IL-4 and IL-5 in worse prognosis patients rather than the mixed Th1/2 found across the whole cohort. Persistently high levels of both Th1 and Th2 cytokines were detected in RP compared to control patients, despite the removal of relatively small tumour burdens. Cytokine expression studies may be useful as surrogate marker of potential disease progression, and could be used to identify patients who may benefit from immune modulation post-surgery.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Bianco Jr FJ, Wood Jr DP, Gomes de Oliveira J, Nemeth JA, Beaman AA, Cher ML . Proliferation of prostate cancer cells in the bone marrow predicts recurrence in patients with localized prostate cancer. Prostate 2001; 49: 235–242.
Shariat SF, Kattan MW, Song W, Bernard D, Gottenger E, Wheeler TM et al. Early postoperative peripheral blood reverse transcription PCR assay for prostate-specific antigen is associated with prostate cancer progression in patients undergoing radical prostatectomy. Cancer Res 2003; 63: 5874–5878.
Okegawa T, Nutahara K, Higashihara E . Detection of micrometastatic prostate cancer cells in the lymph nodes by reverse transcriptase polymerase chain reaction is predictive of biochemical recurrence in pathological stage T2 prostate cancer. J Urol 2000; 163: 1183–1188.
Gao CL, Rawal SK, Sun L, Ali A, Connelly RR, Banez LL et al. Diagnostic potential of prostate-specific antigen expressing epithelial cells in blood of prostate cancer patients. Clin Cancer Res 2003; 9: 2545–2550.
Ferrari MK, McNeal JE, Malhotra SM, Brooks JD . Vascular invasion predicts recurrence after radical prostatectomy: stratification of risk based on pathologic variables. Urology 2004; 64: 749–753.
Ahlering TE, Skarecky DW, McLaren CE, Weinberg AC . Seminal vesicle involvement in patients with D1 disease predicts early prostate specific antigen recurrence and metastasis after radical prostatectomy and early androgen ablation. Cancer 2002; 94: 1648–1653.
Holmberg L, Bill-Axelson A, Helgesen F, Salo JO, Folmerz P, Haggman M et al. A randomized trial comparing radical prostatectomy with watchful waiting in early prostate cancer. N Engl J Med 2002; 347: 781–789.
Karakiewicz PI, Eastham JA, Graefen M, Cagiannos I, Stricker PD, Klein E et al. Prognostic impact of positive surgical margins in surgically treated prostate cancer: multi-institutional assessment of 5831 patients. Urology 2005; 66: 1245–1250.
Ward JF, Slezak JM, Blute ML, Bergstralh EJ, Zincke H . Radical prostatectomy for clinically advanced (cT3) prostate cancer since the advent of prostate-specific antigen testing: 15-year outcome. BJU Int 2005; 95: 751–756.
Pound CR, Partin AW, Eisenberger MA, Chan DW, Pearson JD, Walsh PC . Natural history of progression after PSA elevation following radical prostatectomy. JAMA 1999; 281: 1591–1597.
Potter KJ, Gompels MM, Langkamer VG, Virgo PF, Lock RJ . Th1 and Th2 subsets in orthopaedic surgery by single-cell cytokine analysis. Clin Lab 2003; 49: 197–202.
Menger MD, Vollmar B . Surgical trauma: hyperinflammation versus immunosuppression? Langenbecks Arch Surg 2004; 389: 475–484.
Giraud O, Molliex S, Rolland C, Lecon-Malas V, Desmonts JM, Aubier M et al. Halogenated anesthetics reduce interleukin-1beta-induced cytokine secretion by rat alveolar type II cells in primary culture. Anesthesiology 2003; 98: 74–81.
Yu Y, Zhou Z, Xu J, Liu Z, Wang Y . Ketamine reduces NFkappaB activation and TNF-alpha production in rat mononuclear cells induced by lipopolysaccharide in vitro. Ann Clin Lab Sci 2002; 32: 292–298.
Helmy SA, Al-Attiyah RJ . The effect of halothane and isoflurane on plasma cytokine levels. Anaesthesia 2000; 55: 904–910.
Le Cras AE, Galley HF, Webster NR . Spinal but not general anesthesia increases the ratio of T helper 1 to T helper 2 cell subsets in patients undergoing transurethral resection of the prostate. Anesth Analg 1998; 87: 1421–1425.
McClinton S, Miller ID, Eremin O . An immunohistochemical characterisation of the inflammatory cell infiltrate in benign and malignant prostatic disease. Br J Cancer 1990; 61: 400–403.
Mercader M, Bodner BK, Moser MT, Kwon PS, Park ES, Manecke RG et al. T cell infiltration of the prostate induced by androgen withdrawal in patients with prostate cancer. Proc Natl Acad Sci USA 2001; 98: 14565–14570.
Webster WS, Small EJ, Rini BI, Kwon ED . Prostate cancer immunology: biology, therapeutics, and challenges. J Clin Oncol 2005; 23: 8262–8269.
Groux H, O'Garra A, Bigler M, Rouleau M, Antonenko S, de Vries JE et al. A CD4+ T-cell subset inhibits antigen-specific T-cell responses and prevents colitis. Nature 1997; 389: 737–742.
Shimizu J, Yamazaki S, Sakaguchi S . Induction of tumor immunity by removing CD25+CD4+ T cells: a common basis between tumor immunity and autoimmunity. J Immunol 1999; 163: 5211–5218.
Woo EY, Chu CS, Goletz TJ, Schlienger K, Yeh H, Coukos G et al. Regulatory CD4(+)CD25(+) T cells in tumors from patients with early-stage non-small cell lung cancer and late-stage ovarian cancer. Cancer Res 2001; 61: 4766–4772.
Kono K, Kawaida H, Takahashi A, Sugai H, Mimura K, Miyagawa N et al. CD4(+)CD25(high) regulatory T cells increase with tumor stage in patients with gastric and esophageal cancers. Cancer Immunol Immunother 2006; 55: 1064–1071.
Curiel TJ, Coukos G, Zou L, Alvarez X, Cheng P, Mottram P et al. Specific recruitment of regulatory T cells in ovarian carcinoma fosters immune privilege and predicts reduced survival. Nat Med 2004; 10: 942–949.
Prabhala RH, Neri P, Bae JE, Tassone P, Shammas MA, Allam CK et al. Dysfunctional T regulatory cells in multiple myeloma. Blood 2006; 107: 301–304.
Okita R, Saeki T, Takashima S, Yamaguchi Y, Toge T . CD4+CD25+ regulatory T cells in the peripheral blood of patients with breast cancer and non-small cell lung cancer. Oncol Rep 2005; 14: 1269–1273.
Liyanage UK, Moore TT, Joo HG, Tanaka Y, Herrmann V, Doherty G et al. Prevalence of regulatory T cells is increased in peripheral blood and tumor microenvironment of patients with pancreas or breast adenocarcinoma. J Immunol 2002; 169: 2756–2761.
Friberg D, Bryant J, Shannon W, Whiteside TL . In vitro cytokine production by normal human peripheral blood mononuclear cells as a measure of immunocompetence or the state of activation. Lab Immunol 1994; 1: 261–268.
Tabuchi Y, Shinka S, Ishida H . The effects of anesthesia and surgery on count and function of neutrophils. J Anesth 1989; 3: 123–131.
Acknowledgements
We thank Dr Mike Whelan at Onyvax Ltd for his advice and technical support during this research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Quatan, N., Meyer, B., Bailey, M. et al. Persistently high levels of immunosuppressive cytokines in patients after radical prostatectomy. Prostate Cancer Prostatic Dis 9, 420–425 (2006). https://doi.org/10.1038/sj.pcan.4500899
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.pcan.4500899